Clinicopathologic Features of Agranulocytosis in the Setting of Levamisole-Tainted Cocaine/Κλινικοπαθολογικά Χαρακτηριστικά Ακοκκιοκυττάρωσης στη ρύθμιση της Λεβαμισόλης – Νοθευμένη κοκαΐνη
Abstract
Levamisole is a known contaminant of cocaine and, via this route, has been associated with otherwise unexplained agranulocytosis. Levamisole is currently present in the majority of cocaine samples seized by the US Drug Enforcement Agency. We identified 20 cases of unexplained agranulocytosis in our practice locations of Albuquerque, NM, and Vancouver, Canada. Epidemiologic investigation revealed recent or ongoing cocaine use in 14 cases (70%). Certain morphologic features, including circulating plasmacytoid lymphocytes, increased bone marrow plasma cells, and mild megakaryocytic hyperplasia, were associated with the cocaine-exposed group. Of 5 patients tested, 3 (60%) were HLA-B27+ and showed antineutrophil antibodies, consistent with known associations of levamisole-induced agranulocytosis. One patient, who was positive for cocaine and levamisole by toxicology testing, died of infectious complications. Inadvertent consumption of levamisole via cocaine is a severely underappreciated risk factor for agranulocytosis, and specific laboratory features are suggestive of this etiology.
Agranulocytosis, defined as an absolute neutrophil count of less than 500/μL (0.5 × 109/L), places an affected patient at increased risk of morbidity and mortality related to infectious complications. A wide variety of initiating events and pathologic processes can give rise to severe neutropenia and agranulocytosis, including inherited syndromes, drug effect, alloimmune and autoimmune attack, infection, and malignancy. In some cases, however, an initiating cause cannot be identified, rendering the process idiopathic. We report herein that in 2 widely separated locations in North America (New Mexico and British Columbia), a large proportion of otherwise unexplained cases of agranulocytosis occur in patients with known recent cocaine ingestion; moreover, multiple lines of evidence point to the contaminant levamisole as the responsible etiologic agent.
Levamisole, the enantiomer of the synthetic drug tetramisole, is a synthetic imidazothiazole derivative originally formulated as an anthelmintic agent. It found widespread use in the 1970s as an immunomodulatory agent.1,2 Recent applications have also included exploitation of its antineoplastic properties in adjuvant chemotherapeutic regimens, especially for colorectal cancer.2–4 Levamisole remains widely used in veterinary medicine as an anthelmintic agent, particularly in ruminants and hogs.5,6 During the 1970s, a period during which levamisole was more commonly prescribed to humans, agranulocytosis was well recognized as an idiosyncratic reaction, occurring in 3% to 10% of patients exposed to levamisole.7–9
In addition to the applications described, levamisole is also a known contaminant of cocaine.10–12 The percentage of cocaine samples containing levamisole has increased steadily since 2005.12 As of July 2009, the Drug Enforcement Administration (DEA) of the US Department of Justice reported that 69% of cocaine bricks coming into the United States contained levamisole (US Department of Justice DEA, written communication). The high prevalence of levamisole in the cocaine supply has led some to speculate that it may provide a pharmacomodulatory effect.13
Levamisole-tainted cocaine has been reported as a known or suspected etiologic agent in rare cases of otherwise unexplained agranulocytosis13; however, detailed morphologic features were not reported. Given a recent increase in the number of agranulocytosis cases seen in our practice locations, we undertook a collaborative investigation to document the clinical and morphologic features of agranulocytosis associated with cocaine use and possible levamisole ingestion. We report that, in our practices, a majority of otherwise idiopathic agranulocytosis currently arises in the setting of cocaine use and/or unwitting levamisole ingestion and that specific laboratory findings and morphologic characteristics are associated with this phenomenon.
Materials and Methods
Patient Characteristics
After epidemiologic investigation conducted by the New Mexico Department of Health (NMDOH) revealed that cocaine contaminated with levamisole was potentially the cause of agranulocytosis in some idiopathic cases, we searched diagnostic pathology databases at the University of New Mexico (UNM) Health Science Center (Albuquerque), with the approval of the UNM Institutional Review Board, for patients with absolute neutrophil counts less than 500/μL (0.5 × 109/L) and/or a diagnosis of agranulocytosis between January 1, 2008, and January 1, 2009. Corresponding charts were reviewed to rule out clinical situations in which agranulocytosis could be considered an expected finding at initial diagnosis (ie, hematopoietic malignancy, bone marrow failure, chemotherapeutic treatment, and/or therapy with an agent known to be associated with the development of agranulocytosis). Thirteen patients with agranulocytosis of unclear etiology at initial examination were identified, 7 of whom had subsequent episodes of agranulocytosis. Three patients resided outside New Mexico or were seen in consultation from outside New Mexico (1 each from Colorado, Arizona, and Nebraska); all other patients with agranulocytosis seen at the UNM Health Science Center were from New Mexico.
Table 1
Significant Clinical Features of Patients With Agranulocytosis
Field investigations by NMDOH epidemiologists and/or chart reviews conducted by clinicians were used to divide the 13 patients into 2 groups: patients with a documented history of cocaine use preceding the agranulocytosis and patients without a confirmed history of cocaine use. Clinical and morphologic features of 6 additional cases of cocaine-associated agranulocytosis were also identified and reviewed on a prospective basis by the Vancouver Island Health Authority, Vancouver, Canada, during the same period as in New Mexico. The New Mexico Office of the Medical Investigator reported to NMDOH a patient with a history of agranulocytosis 6 months before autopsy in whom postmortem toxicology testing was positive for cocaine Table 1 (case 3). In summary, our sample comprised 14 cases with documented cocaine use and 6 with no documented exposure. Detailed patient characteristics are presented in Table 1.
Morphologic Review
Peripheral blood, bone marrow aspirate, and posterior iliac crest trephine biopsy specimens were available for morphologic review in all agranulocytosis cases, excluding the postmortem case (case 3, peripheral blood only). Cases were reviewed before the administration of granulocyte colony-stimulating factor (GCSF), except for case 10. Slides from all available cases were reviewed by 3 hematopathologists working independently (D.R.C., J.M., and K.F.) and blinded to the cocaine exposure status of the patients. Morphologic data were recorded for each case using a standardized form incorporating all parameters of basic peripheral blood and bone marrow morphologic review, including estimation of cell populations, adequacy of maturation, and dysplastic features. New Mexico cases were reviewed by at least 2 hematopathologists (D.R.C. and K.F.), and 30% of the cases were reviewed blindly by all 3 hematopathologists to ensure accuracy and concordance of the morphologic assessment. When discordance arose, the case was classified according to the majority opinion. When available, immunohistochemical and in situ hybridization results produced in the initial diagnostic workup were also reviewed.
Additional Laboratory Investigation
For the single postmortem cocaine-positive case (case 3), gas chromatography/mass spectrophotometric toxicology testing was conducted by the NMDOH Scientific Laboratory Division to specifically document or exclude the presence of levamisole, according to previously published spectrophotometric characteristics of levamisole.12
Additional material was available for limited additional laboratory analysis in selected cases. Genomic DNA isolated from banked, cryopreserved mononuclear cells from 5 patients Table 2 was used to determine HLA-B genotype via a sequence-specific priming approach (Micro SSP, One Lambda, Canoga Park, CA) according to the manufacturer’s instructions. Antineutrophil antibody testing was performed using cryopreserved plasma samples from 5 patients (Table 2).
Neutrophil antibodies were detected by using a flow cytometric procedure described previously.14,15 In brief, normal donor neutrophils were isolated to more than 95% purity using dextran sedimentation and Ficoll density centrifugation. Neutrophils were incubated with serum in the presence or absence of levamisole (0.250 mg/mL) for 30 minutes at room temperature in wells of a microtiter plate. Wells without drug were then washed 3 times with phosphate-buffered saline/EDTA buffer, and wells containing drug were washed 3 times with buffer containing 0.250 mg/mL of levamisole. After washing, neutrophils were incubated with F(ab’)2 fragments of fluorescein isothiocyanate–goat antihuman IgG and γFc-specific and phycoerythrin–goat antihuman IgM (μ chain–specific; Jackson ImmunoResearch Laboratories, West Grove, PA), and neutrophil-bound fluorescence was measured with a FACSCalibur flow cytometer (Becton Dickinson, San Jose, CA). Serum samples from healthy donors and serum samples containing previously identified neutrophil-reactive antibodies were used as negative and positive control samples, respectively.
Table 2
Significant Clinical and Pathologic Findings in Agranulocytosis Cases
Results
The median age of the patients was 45 years. Of the 20 patients, 14 (70%) were women and 6 (30%) were men. There was a history of cocaine exposure in 14 patients (70%). Epidemiologic field work in 3 non–cocaine-exposed cases identified therapeutic drugs as the likely etiologic agents of agranulocytosis. Viral workup varied by case, but no patients were known or found to be HIV+. In 5 patients (25%), hepatitis C infection had been documented; the patients were not receiving interferon treatment at the time of presentation with agranulocytosis. A majority of the patients had signs of infection, the most common being pharyngitis. The level of neutropenia was severe in that most patients had a nadir absolute neutrophil count of 0/μL. Patients were generally treated with antibiotics, and 17 (85%) received GCSF support to hasten WBC recovery. In 7 patients (35%), there was at least 1 recurrent episode of agranulocytosis, and 1 patient died of infectious complications.
Pertinent morphologic findings are given in Table 3. The following were more frequent in cocaine-exposed than in non–cocaine-exposed cases: microcytosis; toxic neutrophilic granulation; peripheral left shift; increased circulating large granular lymphocytes, activated lymphocytes, plasmacytoid lymphocytes, and immunoblasts; thrombocytosis; mild megaloblastic change in erythroid precursors; prominent primary granules in myeloid precursors; bone marrow plasmacytosis; and increased megakaryocytes. Of these, circulating plasmacytoid lymphocytes, bone marrow plasmacytosis, and megakaryocytic hyperplasia were the morphologic parameters most divergent between cocaine-exposed and non–cocaine-exposed cases. Indeed, at least 2 of 3 of these features were present in 10 (77%) of 13 cocaine-exposed cases and not present in 5 (83%) of 6 non–cocaine-exposed cases.
Table 3
Selected Morphologic Features in Agranulocytosis Cases
For the purposes of this investigation, we considered a plasmacytoid lymphocyte to be a cell with the chromatin pattern of a mature lymphocyte but an eccentric location to the nucleus and a more basophilic tint to the cytoplasm. Marrow plasmacytosis and megakaryocytic hyperplasia were subjective judgments based on the totality of the morphologic evidence in bone marrow aspirate smears and bone marrow biopsy sections. For the New Mexico cases, concordance among hematopathologists was reached in 11 (79%), 13 (93%), and 14 (100%) of 14 cases for presence or absence of plasmacytoid lymphocytes, marrow plasmacytosis, and megakaryocytic hyperplasia, respectively.
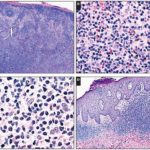
When present, plasmacytoid lymphocytes represented a minority of the circulating lymphocytes. The extent of bone marrow plasmacytosis varied significantly, with some cases showing only a minimal increase in plasma cells and others demonstrating marked polyclonal plasmacytosis comprising up to 30% on differential counts Image 1. Of note, the plasma cells were absolutely increased, often in the setting of a relatively preserved cellularity, rather than only relatively increased in a hypocellular marrow. Plasma cells in cocaine-exposed cases were more frequently large with binucleation and Russell bodies. When present, megakaryocytic hyperplasia was mild, with slight megakaryocytic clustering and a wide range in megakaryocyte size Image 2.
As depicted in Table 3, 3 (60%) of 5 tested patients were HLA-B27+, while 3 (60%) of 5 tested patients had IgG or IgM antineutrophil antibodies in their acute serum samples Figure 1. These antibodies recognized normal donor neutrophils, and binding was not dependent on the presence of levamisole.
Retrospective review of the mass spectrophotometric toxicology spectra for case 3 revealed the presence of cocaine and levamisole in the patient’s postmortem blood sample obtained at the time of autopsy.
Discussion
We report that in a 12-month period in 2 geographically and ethnically diverse populations, the majority of cases of agranulocytosis without clear etiologic explanation arose in patients with a recent history of cocaine use. Prior published reports from a third location (Alberta, Canada) of 5 cases of agranulocytosis in the setting of the use of levamisole-tainted cocaine13 raise suspicion that this phenomenon may be operative at a currently unknown incidence across North America and perhaps beyond.
Image 1
| A bone marrow clot section stained for CD138 expression shows plasmacytosis (×100). Increased bone marrow plasma cells were frequently seen in the cocaine-exposed group. The plasma cells in all cases were polytypic by flow cytometry and/or in situ hybridization for κ and λ light chain expression. |
Figure 1
| Flow cytometric test results for serum IgM (A) and IgG (B) antibodies against neutrophils. Serum samples from patients exposed to levamisole were tested against normal target neutrophils in the presence (data not shown) and absence of levamisole. IgM and IgG antibodies reactive with neutrophils were detected using phycoerythrin (PE)-labeled goat antihuman IgM and IgG. Serum from healthy persons (lanes 1 and 2) served as negative controls, and human serum with neutrophil antibodies against the CD177 protein served as positive control (lane 6). Results for cases 2, 4, and 14 are shown in lanes 3, 4, and 5, respectively. Median fluorescence intensity values are shown above each histogram. A, Serum samples in all 3 cases had strong IgM neutrophil antibody reactivity. B, Case 4 and 14 had IgG neutrophil antibody reactivity. The serum sample in case 2 showed negative results. |
Image 2
| A bone marrow trephine biopsy sample showing megakaryocytic hyperplasia in a cocaine-exposed patient with agranulocytosis. Megakaryocytic hyperplasia was identified more frequently in cocaine-exposed agranulocytosis cases than in nonexposed cases. The megakaryocytes represented a full spectrum of morphologic types, with small and large megakaryocytes of variable lobation identifiable (H&E, ×200). |
We find strong, circumstantial support for the hypothesis that the contaminant levamisole is the responsible agent in our cases. The high rate of detection of levamisole in cocaine samples by the DEA demonstrates significant population-wide exposure in cocaine users. In combination with the marked overrepresentation of cocaine users in the pool of patients with idiopathic agranulocytosis, this finding is highly suggestive of an etiologic role for levamisole, especially because cocaine itself is not known to cause agranulocytosis. In addition, we report 1 case (case 3) in which levamisole was directly detected, along with cocaine, in a blood sample from a patient with a history of agranulocytosis.
The clinical characteristics of the cocaine-associated cases match the pattern established in prior investigations of levamisole-induced agranulocytosis. In the 1970s, a strong association was recognized between the HLA-B27 genotype and susceptibility to levamisole-induced agranulocytosis.16 Prior reports describe HLA-B27 as present in 33% to 50% of cases of levamisole-associated agranulocytosis.16,17 In our series, 3 (60%) of 5 patients with cocaine-associated agranulocytosis for whom testing could be performed were HLA-B27+; in contrast, the local population frequency of HLA-B27 is 8.5% (L. Voit, TriCore Reference Laboratories, Albuquerque, verbal communication, May 15, 2009). Thus, our data show the genotypic susceptibility previously described in agranulocytosis following levamisole exposure. A central role for specific HLA molecules in certain drug hypersensitivity reactions is well described,18 although the mechanism of HLA-B27 in levamisole-associated agranulocytosis requires further investigation.
The plasmacytic proliferations are consistent with previous studies suggesting that levamisole induces agranulocytosis via an antibody-mediated process. Indeed, we were able to document the presence of antineutrophil antibodies in 3 (60%) of 5 patients in the cocaine-exposed group. These antibodies were directed against antigens borne on the surface of normal donor neutrophils and were capable of binding in the absence of levamisole. These findings are directly analogous to those of prior investigators who detected granulocyte-agglutinating or granulocytotoxic antibodies in 25% to 100% of levamisole-associated agranulocytosis.9,16,19–23 The exact mechanism by which such antibodies are formed is unclear, although the dispensability of the presence of the drug for antigen binding may suggest cross-reactivity rather than a hapten-mediated process.
A systematic, blinded review of the morphologic features of cocaine-associated and non–cocaine-associated idiopathic agranulocytosis reveals that circulating plasmacytoid lymphocytes, increased bone marrow plasma cells, and megakaryocytic hyperplasia are important parameters for the discrimination of cocaine-exposed and non–cocaine-exposed cases of agranulocytosis. The presence or absence of at least 2 of these features permits the discrimination of most cocaine-exposed and non–cocaine-exposed cases in our sample population. However, it is important to note that the predictive value of such a scheme is highly dependent on the prevalence of the condition, which seems remarkably high in our population. In addition, our data set represents a convenience sample and not a formal case-control study. Despite the extensive epidemiologic field work, the data are ultimately dependent on patient self-reporting of illegal activities, and, therefore, it is possible that some patients in the “nonexposed” group were, in fact, exposed to cocaine. Finally, the presence of hepatitis C infection in 5 patients represents a common comorbidity in the patient population under study and, thus, is difficult to rule out as a confounding variable. However, cytopenias in patients with hepatitis C are usually associated with interferon therapy, which was not ongoing in these cases at the time of agranulocytosis. Therefore, despite these caveats, in the context of otherwise unexplained agranulocytosis, assessment of these morphologic parameters may support levamisole-contaminated cocaine exposure as a possible cause.
It is interesting that antineutrophil cytoplasmic antibodies (cANCAs) were present in 3 of the 4 tested cocaine-associated cases for which testing could be performed. cANCA positivity has also been described in the setting of cocaine use complicated by nasal septal necrosis.24 Thus, it is unclear in our cases whether the cANCA response is etiologically related to cocaine or to levamisole, although one cANCA+ cocaine-exposed patient denied intranasal cocaine use. Regardless, the presence of cANCAs in cocaine-associated agranulocytosis serves to underscore that cANCA positivity alone should not be considered diagnostic of vasculitis and/or Wegener granulomatosis.
Aside from the postmortem case in which cocaine, levamisole, and agranulocytosis coincided, we did not directly document the presence of levamisole in the clinical agranulocytosis specimens. However, as the half-life of levamisole is relatively short (5.6 hours),25 this does not exclude an etiologic role for levamisole adulteration. Clinicians investigating levamisole as a possible agent in cases of agranulocytosis should be aware of the necessity of obtaining samples for toxicology testing as soon as possible after a patient comes to clinical attention.
It is noteworthy that the dosing schedule for levamisole is important in the development of agranulocytosis. Amery and Butterworth8 found that 3.1% of patients given levamisole for 2 consecutive days every week developed agranulocytosis, whereas only 0.1% receiving the drug for 3 consecutive days every other week experienced this effect, suggesting that temporal frequency of exposure in large part determines the severity of the granulocytic insult. We speculate that habitual cocaine use in the affected patients may have approximated the dosing schedule associated with increased risk. Indeed, 4 of the cocaine-exposed patients experienced a relapsing course, and clinical investigation revealed ongoing cocaine use. When administered, GCSF resulted in prompt recovery of the neutrophil count. However, the death of patient 3 of infectious complications in the setting of agranulocytosis, with positive toxicology for cocaine and levamisole, highlights the potential dangers of this phenomenon.
Frequent contamination of cocaine with levamisole represents an underappreciated risk factor for agranulocytosis, and clinical investigation in cases of idiopathic agranulocytosis should include a careful history regarding possible cocaine use. In addition, a constellation of morphologic findings—especially the presence of circulating plasmacytoid lymphocytes, increased bone marrow plasma cells, and increased megakaryocytes—is associated with otherwise unexplained agranulocytosis in this setting and should raise suspicion of levamisole/cocaine-associated agranulocytosis. The HLA-B27 genotype and the presence of antineutrophil antibodies are associated with levamisole-induced agranulocytosis, in the literature and in our case series. These findings may be especially useful for hematopathologists given limited clinical information or for clinicians treating patients unable or unwilling to reveal a history of illicit drug use.
We thank TriCore Reference Laboratories, Barbara Masten, PhD, and Thomas M. Williams, MD, for assistance with HLA typing, and Eugenia Brazwell, PhD, and Michael Crossey, MD, PhD, for assistance with toxicology testing.
Upon completion of this activity you will be able to:
- recognize the high prevalence of the pharmaceutical agent levamisole in the current supply of illegal cocaine in the United States.
- gain awareness that levamisole-contaminated cocaine represents an underappreciated risk factor for agranulocytosis.
- identify morphologic features from peripheral blood and bone marrow that correlate with cocaine use in the setting of unexplained agranulocytosis.
The ASCP is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians. The ASCP designates this educational activity for a maximum of 1 AMA PRA Category 1 Credit™ per article. This activity qualifies as an American Board of Pathology Maintenance of Certification Part II Self-Assessment Module.
The authors of this article and the planning committee members and staff have no relevant financial relationships with commercial interests to disclose.
Questions appear on p 512. Exam is located at www.ascp.org/ajcpcme
Author contributions were as follows: designed research; collected, analyzed, and interpreted data; and wrote manuscript, Dr Czuchlewski; designed research and collected, analyzed, and interpreted data, Ms Brackney and Drs Nolte, Rabinowitz, Baumbach, and Foucar; collected, analyzed, and interpreted data, Ms Ewers, Mr Curtis, and Dr McFarland; collected data, Drs Manna and Fekrazad; analyzed and interpreted data, Dr Martinez; and designed research, Dr Hjelle.
© American Society for Clinical Pathology
David R. Czuchlewski, MD
Monica Brackney, MS
Christina Ewers, MSN
Jonaki Manna, MD
M. Houman Fekrazad, MD
Afton Martinez
Kurt B. Nolte, MD
Brian Hjelle, MD
Ian Rabinowitz, MD
Brian R. Curtis
Janice G. McFarland, MD
Joan Baumbach, MD
Kathryn Foucar, MD