Addiction Treatment With a Dark Side (En)
The Double-Edged Drug
In Demand in Clinics and on the Street, ‘Bupe’ Can Be a Savior or a Menace
| After two years of buprenorphine treatment, Shawn Schneider has rebounded from a self-destructive addiction to painkillers. Leslye Davis/The New York Times |
For Shawn Schneider, a carpenter and rock musician, the descent into addiction began one Wisconsin winter with a fall from a rooftop construction site onto the frozen ground below. As the potent pain pills prescribed for his injuries became his obsessive focus, he lost everything: his band, his job, his wife, his will to live.
Mr. Schneider was staying in his parents’ basement when he washed down 40 sleeping pills with NyQuil and beer. His father heard him gasping and intervened, a reprieve that led Mr. Schneider into rehab, not his first program, but the one where he discovered buprenorphine, a substitute opioid used to treat opioid addiction.
In the two years since, by taking his “bupe” twice daily and meeting periodically with the prescribing psychiatrist, Mr. Schneider, 38, has rebounded.He is sober, remarried, employed building houses, half of a new acoustic duo and one of the many addicts who credit buprenorphine, sold mostly in a compound called Suboxone, with saving their lives.
Suboxone did not save Miles Malone, 20; it killed him. In 2010, a friend texted Mr. Malone an invitation to use the drug recreationally — “we can do the suboxins as soon as I give them to u, iight, dude?” — and he died that night in South Berwick, Me., of buprenorphine poisoning. The friend, Shawn Verrill, was sentenced this summer to 71 months in prison.
“I didn’t know you could overdose on Suboxone,” Mr. Verrill said in an interview at a federal prison in Otisville, N.Y. “We were just a bunch of friends getting high and hanging out, doing what 20-year-olds do. Then we went to sleep, and Miles never woke up.”
Suboxone is the blockbuster drug most people have never heard of. Surpassing well-known medications like Viagra and Adderall, it generated $1.55 billion in United States sales last year, its success fueled by an exploding opioid abuse epidemic and the embrace of federal officials who helped finance its development and promoted it as a safer, less stigmatized alternative to methadone.
But more than a decade after Suboxone went on the market, and with the Affordable Care Act poised to bring many more addicts into treatment, the high hopes have been tempered by a messy reality. Buprenorphine has become both medication and dope: a treatment with considerable successes and also failures, as well as a street and prison drug bedeviling local authorities. It has attracted unscrupulous doctors and caused more health complications and deaths than its advocates acknowledge.
It has also become a lucrative commodity, creating moneymaking opportunities — for manufacturers, doctors, drug dealers and even patients — that have undermined a public health innovation meant for social good. And the drug’s problems have emboldened some insurers to limit coverage of the medication, which cost state Medicaid agencies at least $857 million over a three-year period through 2012, a New York Times survey found.
Intended as a long-term treatment for people addicted to opioids — heroin as well as painkillers — buprenorphine, like methadone, is an opioid itself that can produce euphoria and cause dependency. Its effects are milder, however, and they plateau, making overdoses less likely and less deadly. And unlike methadone, buprenorphine (pronounced byoo-pruh-NOR-feen) is available to addicts by prescription, though only from federally authorized doctors with restricted patient loads.
<http://nyti.ms/17bvpnG< |
|
Video | :42
Ken Mobley, a jailer in Whitley County,
Ky., talking about the problem of Suboxone in prisons. Leslye Davis/The New York Times |
Partly because of these restrictions, a volatile subculture has arisen, with cash-only buprenorphine clinics feeding a thriving underground market that caters to addicts who buy it to stave off withdrawal or treat themselves because they cannot find or afford a doctor; to recreational users who report a potent, durable buzz; and to inmates who see it as “prison heroin” and, especially in a new dissolvable filmstrip form, as ideal contraband.
“It’s such a thin strip they’ll put it in the Holy Bible, let it melt and eat a page right out of the good book,” said Ken Mobley, a jailer in Whitley County, Ky., who randomly screened 50 inmates recently and found 21 positive for Suboxone.
Many buprenorphine doctors are addiction experts capable, they say, of treating far more than the federal limit of 100 patients. But because of that limit, an unmet demand for treatment has created a commercial opportunity for prescribers, attracting some with histories of overprescribing the very pain pills that made their patients into addicts.
A relatively high proportion of buprenorphine doctors have troubled records, a Times examination of the federal “buprenorphine physician locator” found. In West Virginia, one hub of the opioid epidemic, the doctors listed are five times as likely to have been disciplined as doctors in general; in Maine, another center, they are 14 times as likely.
Nationally, at least 1,350 of 12,780 buprenorphine doctors have been sanctioned for offenses that include excessive narcotics prescribing, insurance fraud, sexual misconduct and practicing medicine while impaired. Some have been suspended or arrested, leaving patients in the lurch.
Statistics released in the last year show sharp increases in buprenorphine seizures by law enforcement, in reports to poison centers, in emergency room visits for the nonmedical use of the drug and in pediatric hospitalizations for accidental ingestions as small as a lick.
Buprenorphine’s staunchest proponents see these indicators as a byproduct of the drug’s rising circulation and emphasize its safety relative to other opioids.
“The benefits are high, the risk is low and it is worth it on a population-wide basis,” said Dr. Stuart Gitlow, the president of the American Society of Addiction Medicine.
But Dr. Robert Newman, a leading advocate of methadone treatment, said, “The safety factor should not be oversold.”
“It is diverted and sold on the black market,” he said. “It is misused, and it does lead to medically adverse consequences, including death. It is associated with a large number of deaths.”
The addiction drug was a “primary suspect” in 420 deaths in the United States reported to the Food and Drug Administration since it reached the market in 2003, according to a Times analysis of federal data.
But buprenorphine is not being monitored systematically enough to gauge the full scope of its misuse, some experts say. The Centers for Disease Control and Prevention does not track buprenorphine deaths, most medical examiners do not routinely test for it, and neither do most emergency rooms, prisons, jails and drug courts.
“I’ve been studying the emergence of potential drug problems in this country for over 30 years,” said Eric Wish, the director of the Center for Substance Abuse Research at the University of Maryland. “This is the first drug that nobody seems to want to know about as a potential problem.”
The government has a vested interest in its success.
The treatment is the fruit of an extraordinary public-private partnership between a British company and the American government, which financed clinical trials and awarded protection from competition after the drug’s patent expired.
The company, now a consumer goods giant called Reckitt Benckiser, hired several federal officials who had shepherded the drug, and it has financially supported many of the scientists and doctors who are studying it and advocating its use. But over the last few years, the company’s aggressive campaign to protect its lucrative franchise has alienated some of its customers and allies.
In an 11th-hour bid to thwart generic competition and dominate the market with its patent-protected Suboxone filmstrip, the company sought to convince regulators that the tablet form, which earned it billions of dollars, now presented a deadly risk to children as packaged in pill bottles.
The F.D.A. did not agree. Early this year, it approved generic tablets and asked the Federal Trade Commission to investigate potentially anticompetitive business practices by the company.
Reckitt Benckiser defended its advocacy for the Suboxone filmstrip — now its only pharmaceutical product — saying its research showed that the film was safer than the tablets, kept addicts in treatment longer and had less of a street presence. It added that it was overseeing an F.D.A.-required “risk evaluation and mitigation strategy to promote the appropriate use of buprenorphine with the goal to minimize the misuse, abuse and multidose unintentional exposure of these products.”
Dr. John Mendelson of San Francisco, a consultant for the company, said it could be proud of its management of a difficult product. “Their biggest success so far,” he said, “is that the whole system has not imploded, that enough doctors have prescribed the drug appropriately that there has been no move to withdraw it from the market.”
Ronni Katz, a health official in Portland, Me., is less impressed.
“I remember the early days when we met with the pharma rep in the area — I don’t think he was trying to mislead us — he truly believed it was a miracle drug,” she said. “But they way underestimated the potential for abuse, which means to me they really don’t understand addiction.”
Skeptics and Believers
Nearly a half-century ago, buprenorphine was born in the laboratory of an English company specializing in mustard and shoe polish, where chemists were competing to invent a less addictive painkiller.
“We were trying to beat morphine, not methadone,” said John W. Lewis, 81, who oversaw the drug’s development.
Though far more potent than morphine, buprenorphine appeared in animal tests to be unusually safe even in very high doses. In 1971, Dr. Lewis and colleagues traveled to an infirmary in Glasgow to conduct the first human tests — on themselves.
Buprenorphine made Dr. Lewis violently ill. “It quite took the edge off our stay in a splendid hotel on the banks of Loch Lomond,” he said in a speech, and it exposed the painkiller’s “Achilles’ heel” — “the rather high incidence of nausea and vomiting.”
In the mid-1970s, Dr. Lewis began shipping the drug to the United States Narcotic Farm in Lexington, Ky., to test its abuse potential on detoxified addicts. A prison that doubled as a treatment hospital, the farm was home to the government’s Addiction Research Center (and at times to jazz greats like Chet Baker, Elvin Jones and Sonny Rollins).
With opposition to human research mounting, buprenorphine would be the last drug tested there; government scientists justified the research by arguing that the painkiller also had the potential to treat addiction.
“Here’s the thing: The Lexingtonians were against methadone,” said Nancy Campbell, a historian of drug policy. “They felt like addicts liked it too much, and it had overdose potential. They never thought abstinence and ‘Just Say No’ would work with this population. So they were eager to find an alternative.”
The idea of using opioid substitutes to treat opioid dependence is based on the premise that long-term drug use profoundly alters the brain, that the craving, seeking and taking of opioids is a “bio-behavioral” compulsion. While addiction is considered a chronic, relapsing disease, experts believe that replacing illegal drugs with legal ones, needles with pills or liquids and more dangerous opioids with safer ones reduces the harm to addicts and to society.
<http://nyti.ms/1dENwDy< |
|
Video | 1:40
Dr. Andrew Kolodny describing how
buprenorphine works. Leslye Davis/The New York Times |
Like heroin, buprenorphine attaches to the brain’s opioid receptors, but it does not plug in as completely. It is slower acting and longer lasting, attenuating the rush of sensation and eliminating the plummets afterward. Addicts develop a tolerance to its euphoric effects and describe themselves as normalized by it, their cravings satisfied. It also diminishes the effects of other opioids but, studies have shown, does not entirely block them, even at the highest recommended doses.
A devoted cadre of government scientists saw buprenorphine as a “holy grail” and over the next few decades “floated in between the public and private sector for most of their careers,” Dr. Campbell said. The farm’s pharmacist would become an executive vice president of Reckitt Benckiser Pharmaceuticals, for example, and the company would contract with the former National Institute on Drug Abuse director who originally promoted the public-private partnership.
It was a collaboration that the company, whose brand names include Lysol, resisted for a long time, said Charles O’Keeffe, a former White House drug policy official who incorporated Reckitt in the United States.
“They were grocers,” he said. “Finally, I went to the board and said, ‘It’s for the social good.’ Ultimately, they relented but said, ‘Just don’t spend a lot of money.’ “
He did not have to. The federal drug abuse institute financed the two big clinical trials necessary to win F.D.A. approval for $28 million and later spent an additional $52.4 million for studies at its clinical research sites. At least $19 million more in studies are underway.
Further, the F.D.A. granted the company a seven-year monopoly based on its claim that it would never recoup its development costs. (Reckitt now has a market value of $56.7 billion; 21 percent of its operating profits last year came from Suboxone.)
Still, hurdles had to be cleared.
First, Mr. O’Keeffe said, “We had to change the law because it would have been illegal.”
The Harrison Narcotics Act of 1914, as interpreted, prohibited doctors from prescribing narcotics to narcotics addicts “to maintain their addictions.” In the 1970s, methadone treatment was authorized but limited to clinics where the drug was dispensed, usually daily.
The original advocates of buprenorphine, though, wanted to make addiction treatment mainstream rather than segregate addicts in clinics that became lightning rods for community opposition. They wanted doctors in offices to prescribe it, just like any other take-home medication.
So Mr. O’Keeffe found “influential members of Congress interested in doing this”: Senators Carl Levin, Democrat of Michigan, and Orrin G. Hatch, Republican of Utah, with support from Senator Joseph R. Biden Jr., Democrat of Delaware. In the end, because of law enforcement concerns, the Drug Addiction Treatment Act of 2000 included unique prescribing restrictions: that doctors seek federal permission, get eight hours of training, accept a 30-patient limit and attest to their ability to make counseling referrals.
The concerns grew from other countries’ experiences with buprenorphine treatment over the previous decade; successes had been accompanied by abuses. So F.D.A. officials insisted on the addition of an “abuse deterrent” — naloxone. If addicts crushed and injected the tablets, the naloxone would precipitate excruciating withdrawal symptoms.
The Drug Enforcement Administration was skeptical, saying studies showed that naloxone did not provoke “any evidence of withdrawal” in “a substantial percentage” of opiate abusers, and that the amount in the proposed compound would produce only a half-hour of “unpleasantness” in those susceptible.
Skeptical, too, were buprenorphine’s original champions at Reckitt, who would have preferred a different additive or more naloxone. “It was not a perfect solution,” Dr. Lewis said.Even so, Suboxone — four parts buprenorphine, one part naloxone — was created. And in late 2002, along with Subutex (plain buprenorphine), it was approved by the F.D.A. just as its target audience was about to expand unexpectedly.
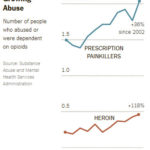
An estimated 2.5 million Americans were dependent on or abused opioids last year, mostly painkillers, although heroin dependence has skyrocketed, with the number of addicts doubling over a decade to 467,000, government data indicate. In 2010, the last year studied, 19,154 people died of opioid overdoses.
“Had buprenorphine never been released and all we had was methadone, that number would be much higher,” said Dr. Andrew Kolodny, the president of Physicians for Responsible Opioid Prescribing.
Early Successes
In the early days of Suboxone, with Reckitt Benckiser barely marketing its own drug, Dr. Kolodny, then a New York City health official, crisscrossed the city with colleagues to spread the word about the new medication, entice public hospitals to try it with $10,000 rewards and urge doctors to get certified.
“We had New York City staff out there acting like drug reps,” Dr. Kolodny said.
He himself became a prescriber. “All of a sudden, I started getting calls from white kids on Long Island who were all addicted to pain pills,” he said. “It was 2003 or 2004, and my first experience of the painkiller epidemic.”
A psychiatrist accustomed to the slow, subtle effects of antidepressants and mood stabilizers, Dr. Kolodny was stunned by patients who arrived “a total mess” and in days seemed “back to normal.”
“I’m thinking, this cures all addictions,” he said.
Dr. Jeffrey T. Junig of Wisconsin experienced a similar revelation. He was concerned that buprenorphine would create “all these dry drunks, people who were no longer using but who hadn’t addressed their defects.” Instead, he witnessed something different: “The process of craving opioids itself causes people to be so one-dimensional that it is a defect itself. Freed from the obsession to use, people change.”
Buprenorphine worked so well on his first patients, middle-aged painkiller addicts, that “they would have tears rolling down their faces talking about how grateful they were,” he said.
<http://nyti.ms/17dBW14< |
|
Video | 1:10
Mr. Schneider worries that the misuse of
buprenorphine could hurt those who use it legitimately. Leslye Davis/The New York Times |
Among them was Shawn Schneider, who had found his way to Dr. Junig after swallowing 400 milligrams of Ambien, thinking, “If I wake up, I wake up; if I die, I die.”
Like Mr. Schneider, dozens of addicts interviewed portrayed themselves as exhausted and frightened before they started on Suboxone. They acknowledged having “loved” their chosen opiate but not what turned into a miserable existence dominated by drug-seeking to avoid “dope sickness.”
Travis Norton, 33, gravitated to heroin in adolescence as a result of a misguided infatuation with artist addicts like William S. Burroughs and Kurt Cobain, he said. For years, he cycled through costly abstinence-based programs, always returning to the needle.
“I was a chronic relapse,” said Mr. Norton, who is now an addiction counselor in a Minneapolis suburb. “I was a wreck until I started maintenance therapy in 2003. And I’ve been great since.”
Mr. Norton switched for a time to methadone when his Suboxone doctor retired. At that point, Suboxone, around $16 for an average daily dose, was considered “the rich man’s methadone.” Mr. Norton, not rich but a college-educated professional, found the methadone clinic “a ball and a chain.”
“I had to travel for my job, and there was zero flexibility,” he said. “They had thousands of clients, and I was a number.”
Dr. Edwin A. Salsitz of Beth Israel Medical Center in New York, who has been treating addiction for decades, said that in the pre-Suboxone universe, he encountered all too many middle-class addicts who refused to set foot in a clinic.
“And then sometimes, a couple of years later, they’d be H.I.V. positive, or something more catastrophic would have occurred,” he said. “There’s no way to explain what this meant to the addiction field to have another option besides the clinics.”
Reckitt Benckiser gradually built a stable of doctors paid to advocate use of the treatment, Dr. Salsitz among them.
The recruiting was tough. The recruiting was tough. Those outside the addiction field were reluctant to deal with the hassles of certification, potential visits by the D.E.A. and the addicts themselves. Within the field, buprenorphine faced stiff opposition from the methadone industry as well as traditional rehabilitation programs and the Alcoholics Anonymous movement, which promotes abstinence.
| Melissa Iverson, a 48-year-old former social worker living in Central Florida, said her painkiller addiction had made her go “crazy out of control” until she began taking Suboxone. Leslye Davis/The New York Times |
“With Suboxone, there is a lot of misinformation out there, and the most common is you’ve replaced one drug with another,” said Melissa Iverson, a 48-year-old social worker who lives in Florida and is now on disability because of fibromyalgia.
Ms. Iverson first requested anonymity, like most other professionals interviewed, some of whom have never acknowledged their problem to their families, primary care physicians or even insurers. Eventually she decided to “come out of the closet,” saying, “The stigma needs to be tackled by real people with real names, or else it will haunt us forever.”
Relying on ever-escalating doses of painkillers to cope with her chronic pain, she had gone “crazy out of control.” Her life revolved around pills; she would pass out smoking in bed and wake up with burns on her hands or get into car accidents and nod out in the tow truck. Four years ago, she had “a psychotic break,” ended up hospitalized and “came out on Suboxone.”
In contrast to her painkiller use, she has taken Suboxone at increasingly lower doses, finding that it alleviates her pain without “those self-destructive behaviors.”
“As an addict, I was high all the time,” she said. “With Suboxone, I developed a tolerance within a week. There’s zero euphoria.”
Successes like hers multiplied until demand outstripped supply because of the limited number of doctors and the patient cap. This brought some unintended consequences.
<http://nyti.ms/HSwveC< |
|
Video | 1:37
Ms. Iverson on her addiction and how Suboxone
has helped her recovery. “I could think again, “she said. “I could smile again.” Leslye Davis/The New York Times |
First, some prescribers pushed patients off the medication prematurely to replace them with new patients because the early treatment phase was more lucrative. Second, patients began sharing the drug, trading it and selling it. Buprenorphine trickled out onto the street.
Health officials, concerned about restricted access, lobbied alongside Reckitt Benckiser for the patient cap to be raised. “Why should we bind a healer’s hands from helping as many as he or she could?” Senator Hatch said, getting an amendment passed in 2006 that allowed doctors, on request, to go from 30 to 100 patients after a year.
The stage was set for more patients, prescriptions and problems. “It’s when the limit was raised from 30 that doctors started to get commercial about it,” said Dr. Art Van Zee, whose buprenorphine program at a federally funded community health center in rural Virginia is surrounded by for-profit clinics where doctors charge $100 for weekly visits, pulling in, he estimated, about $500,000 a year.
“They are not savvy about addiction medicine, don’t follow patients very closely, don’t do urine testing and overprescribe,” he said. “That’s how buprenorphine became a street drug in our area.”
Troubled Histories
In Fond du Lac, Wis., on the shores of Lake Winnebago, addicts come and go from a bland building housing a medical office, a cheese business and a title company. They bring their tumultuous lives into a tranquil space with hunter green walls, heathered carpet and easy-listening music, presided over by Dr. Junig’s wife, Nancy, candy jar by her side.
Fond du Lac Psychiatry is the kind of setting the original idealists envisioned. They did not foresee the buprenorphine mega-clinics that resemble and frequently double as painkiller pill mills, sometimes with armed guards to protect their cash.
They did not foresee a buprenorphine empire like the one Dr. Thomas E. Radecki, 67, built in northwestern Pennsylvania.
According to the evidence presented to a grand jury this summer, Dr. Radecki operated four clinics under the business name Doctors and Lawyers for a Drug-Free Youth, serving 1,000 people, many of whom did not need or use buprenorphine and resold it in their neighborhoods. To override the patient limit, he employed other doctors part time. He sold the drug directly to patients, which is legal, and was the country’s largest individual buyer of buprenorphine in the first half of last year, according to investigators. The previous year, he netted $280,000 in profits from the tablets alone, they said.
In August, the Pennsylvania attorney general announced Dr. Radecki’s arrest on charges of improper prescribing and trading addiction drugs for sex. His lawyer, John Froese, said Dr. Radecki “denies that he ever prescribed any medicine that was not helpful to his patients” or had sexual relationships with his buprenorphine patients.
Dr. Radecki lost his Illinois license for just such a relationship, and his Pennsylvania license was made probationary in 2007. Nonetheless, the federal government subsequently authorized him to prescribe buprenorphine and then expand his patient load.
“Very few if any” doctors are denied permission unless they are “under investigation or something pops up,” said Rusty Payne, a D.E.A. spokesman.
The Times analyzed the disciplinary records of the doctors on the federal government’s online listing of buprenorphine providers, which is not comprehensive because doctors can opt out, and calculated state-by-state disciplinary rates.
In 30 of the 31 states that provided their overall disciplinary rates for comparison, buprenorphine doctors are far more likely to have been sanctioned than doctors over all. In Florida and Kentucky, they are four times as likely to have been sanctioned. In New York, they are six times as likely; in Arizona, seven times; in Minnesota, nine times; and in Louisiana, 10 times.
Rates are even higher for the subset certified to treat the maximum patient load, The Times found in analyzing records from a sampling of states.
In Ohio, nearly 17 percent have disciplinary records, compared with 1.6 percent of all doctors. They include individuals sanctioned for: amphetamine addiction coupled with a Medicaid-fraud conviction; conducting an “excessive number of invasive procedures”; smuggling steroids from Mexico; engaging in conversations regarding a “murder for hire” and neglecting to report the rape of a pediatric patient; “digitally penetrating” patients and having sexual intercourse with them in the office.
Some were reprimanded or placed on probation before becoming Suboxone doctors; others, stripped of their licenses recently, had their offices shuttered.
This adds to the volatility of the treatment culture.
A 30-year-old Michigan woman said she was invited into treatment by a doctor who frequented the strip club where she was a bartender and who paid for her medication for several months. When he was placed on probation for “violation of duty/negligence” unrelated to her, she switched to a second doctor, who also got in trouble. After that, the woman bought her buprenorphine on the street for a year — saving $5,500 in medical and counseling fees, she noted — until she found an addiction specialist with an opening.
In some areas, like New York City, there is almost a glut of buprenorphine prescribers. In others, specialists routinely turn away addicts begging for help.
Non-specialists pick up the slack.
Reckitt Benckiser recruited “any doctor willing,” said one former company drug representative who asked not to be identified to protect her career. Those in her territory ranged from “extremely passionate” to intensely commercial, she said: “One charged a $50 co-pay, and another $500 for an initial visit. I had a few physicians using the medication themselves. One guy was so enthusiastic I signed him up as a treatment advocate, but then it turned out he relapsed and lost his license.”
Just because doctors have disciplinary histories does not mean that they are unscrupulous. Some of the most knowledgeable, compassionate addiction doctors are former addicts themselves, with medical board actions on their records that sometimes limit their career options.
| Dr. Jeffrey T. Junig, an anesthesiologist who retrained as a psychiatrist after his own recovery from addiction, never expected to become a buprenorphine doctor. Leslye Davis/The New York Times |
Dr. Junig, 53, is an anesthesiologist with a doctorate in neurochemistry who retrained as a psychiatrist after his own recovery from addiction. He did not intend to become a b